| Item | Price | Qty | Total | |
|---|---|---|---|---|
 Loading Cart...
Loading Cart...Platelet-Rich Plasma Stays Quietly Popular Despite Neglect
According to research, Platelet Rich Plasma (PRP) treatments are one of the most desired treatments available in healthcare. This is notable considering the following:
- The costs of PRP treatments are actually rising. In 2006, you could get a PRP treatment for $450. Today, the cost may be as high as $1,500 (depending on where you get it and what it’s for).
- PRP is not reimbursed by the insurance companies. So, getting patients to pay is hard, especially for a treatment that has the potential for misuse.
- Areas of the medical industry do not support PRP. No big pharma funding on extensive research or marketing. No medical associations lobbying to raise its awareness.
However, we believe the best of PRP is not even here yet. It’s estimated that Asia-Pacific will have the fastest-growing—and a promising—PRP market.
Strongly Based on Fundamental Healing Theory
The growth can be attributed to PRP's fundamental healing property. More platelets mean more growth factors and cytokines, and therefore more healing. It's as simple as that. Our body's natural healing mechanism operates with 150,000/ul-350,000/ul platelets in the blood. Using Platelet-Rich Plasma means this number is amplified by 3X to 5X.
How can this be not translated into better healing?
Believe it or not, the best orthopedic doctors use Platelet-Rich Plasma, and do so regularly.

PRP can be used to promote healing of injured tendons, ligaments, muscles, and joints It can also be applied to address various Aesthetic problems. Researchers conduct regular studies to test its effectiveness.
One landmark study involved double-blind randomized controlled trials to study the effect of PRP on patients with chronic low back pain caused by damaged discs. The study outcome showed that 60% of the patients felt significant improvement. Some even felt they were cured!
Platelet-Rich Plasma Compositions / Variants
Listed below are some of the different PRP compositions :
- Plasma Rich in Growth Factors (PRGF)
- Plasma Rich in Platelets and Growth Factors (PRPGF)
- Platelet-Rich Plasma (PRP); Platelet Poor Plasma (PPP)
- Plasma Rich in Platelets and Rich in Leukocytes (LR-PRP)
- Plasma Rich in Platelets and Poor in Leukocytes (LP-PRP)
- Platelet-Rich Fibrin Matrix (PRFM)
All of them involve separation – Centrifugation is the process used to separate the platelets from the red blood cells. However, what happens after that can vary, and the industry hasn't found its middle ground as to which can be standardized. We believe the confusion will clear up soon.

No matter which variant you end up using, the following bio-factors are at play:
- Growth Factors: TGF-B, PDGF, IGF-I,II, FGF, EGF, VEGF, ECGF
- Adhesive Proteins: Fibrinogen, Fibronectin, Vitronectin, Thrombospondin-1
- Clotting & Anti-Clotting Factors: Proteins, Antithrombin, Plasminogen, Proteases, Antiproteases
How Platelet-Rich Plasma Actually Works
Why is PRP commonly used for wound healing and pain management?
The answer is because the platelets' main job is to trigger coagulation, act as a biologic glue, and support stem cell or primary cell migration.
In addition, PRP also helps in restoring hyaluronic acid, accelerating the synthesis of collagen and glycosaminoglycans, plus heightening the cartilage matrix. Not only that, but the platelets are responsible for clot formation, meaning they can immediately act as a scaffold to stimulate the healing cascade.
95% of the bioactive proteins in PRP are released within 1 hour of injecting Platelet-Rich Plasma. The platelets continue to release growth factors for 7-10 days. Thus, it is sometimes recommended to re-inject PRP every 7 days.

Why Are Patients Spending Their Hard Earned Money For This?
This reminds us of hundreds of thousands of PRP treatments paid for out of the patient's own pocket, even though they've been paying for years to get coverage from their insurance provider.
Today, PRP costs can be anywhere between $500 and $1,500 per site per treatment (depending on where in America the PRP is offered). Most patients opt for repeated treatments! So why are they willing to spend their hard-earned money if the treatment isn’t working? Are there no better alternatives under the "coverage" of their insurance provider? The answer is 1) the treatment works 2) there’s nothing else out there that's as natural with little or no side-effects as with PRP treatments.
Consider the case of osteoarthritis. In 2016, 27 million Americans were impacted by arthritis – 33.6% of the U.S. population over the age of 65 were diagnosed. All of them experienced gradual degeneration of cartilage and bones – with cartilage loss of roughly 5% per year. Yet our medical industry doesn't have a “fix” to stop it. However, when physicians started using PRP treatments for their osteoarthritis patients, they found that a large majority of them had no further cartilage loss. Perhaps it means that PRP treatments should be considered the default first-line of treatment for osteoarthritis nationwide.
Another huge market is hair loss and cosmetic facial applications. Many people may believe that PRP does not work well for hair restoration. Here's one study on the effect of PRP for hair loss:
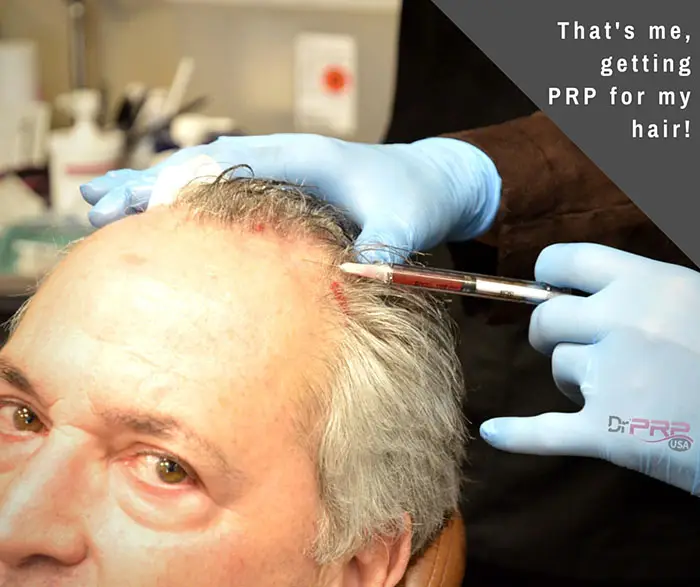
"Hair loss reduced, and at 3 months, it reached normal levels. Hair density reached a peak at 3 months (170.70 ± 37.81, P < 0.001). At 6 months and at 1 year, it was significantly heightened, 156.25 ± 37.75 (P < 0.001) and 153.70 ± 39.92 (P < 0.001) respectively, compared to baseline. Patients were satisfied with a mean result rating of 7.1 on a scale of 1-10. No remarkable adverse effects were noted.” I'll take that. That's me getting PRP for hair. :)
PRP Market Is Projected to Hit $297.6 Million in 2021
Consider this just for osteoarthritis alone. Today, the CDC estimates that over 32.5 million American adults experience osteoarthritis. If every one of these adults received 1 PRP shot a year at a conservative $400 per treatment, it would be a market of $13 billion. And that's one condition out of the many that PRP injections are being used to treat.
Just getting Platelet-Rich Plasma covered by insurance will unleash the market tremendously and may help heal millions of patients naturally and effectively. Perhaps the insurance companies would rather pay for an injection series as opposed to surgery. Why wouldn’t they?
If this treatment could reduce expensive surgical intervention, then it may actually be a wise business decision for the insurance companies in terms of savings. It may only be a matter of time before insurance companies start realizing their folly of not supporting this treatment.
After All Is Said and Done, It's Still "Unproven"
The beauty of PRP is that it can be used for just about everything that needs healing assistance…. and new uses are cropping up quite often! The problem is, these treatments are customized and difficult to standardize because everyone’s blood profile is unique to them. It may be for this reason that PRP is classified as unproven or experimental by the insurance companies.
The VAST scope of PRP calls for urgent structure and guidelines. There are some 20+ conditions where researchers have found it to be of “help” in one way or another. It's a daunting task to prove PRP’s efficiency in all of these areas.
Nevertheless, we will one day get there, though lots of funding is necessary for that to happen. And yes, standardization of PRP composition might help, as well as formulating optimized protocols for each condition. Big pharma will never jump in because there is nothing in it for them!
It's So Simple, You'd Be Foolish Not To Try It
You only need a user friendly phlebotomy system like what we offer here, a proper centrifuge for the kit, and off the shelf needles and syringes
The only complexity comes from not having a suitable PRP system as the final platelet count can depend on a variety of factors, such as the initial volume of blood, technique used and dynamics of the processing kit. On the patient's side, there are factors such as age and general health.
When it comes to platelet concentration, there's often confusion. What is the proper concentration for a therapeutic dose? Is it best to include or exclude leukocytes? What about RBCs….include or exclude? The answer is, it all depends on the tissue you are targeting and the type of injection for which you are preparing.
Although the outcome is not always guaranteed, the correct amount of platelets, platelet activation, and cytokine release, you can begin to get consistency in your PRP outcomes. There is still some uncertainty regarding the number of injections, timing, and delivery method of Platelet-Rich Plasma. But with wide-spread adoption, some guidance is beginning to emerge.
It’s estimated that about 600,000 total knee replacements happen each year. At about $50,000 per replacement, that market would generate around $30 billion. How many of these patients had the good fortune of having their physicians recommend that they try PRP early on?



