| Item | Price | Qty | Total | |
|---|---|---|---|---|
 Loading Cart...
Loading Cart...Advanced Ophthalmic Care: PRP Eye Drops for Superior Ocular Health

Our eyes are our window to the world. But ocular health extends far beyond seeing clearly. Ocular discomfort in the form of dry eyes can make daily life irritating and uncomfortable.
Dry eye disease occurs when the eyes are unable to produce and retain the lubrication necessary for ocular health. There are many different factors that can lead to a decreased production of tears, including:
- Aging
- Autoimmune disease
- Allergic eye disease
- Vitamin A deficiency
- Medications including antihistamines, decongestants, antidepressants, and medications for Parkinson’s disease, birth control, acne, and high blood pressure
- Sensitivity of the corneal nerve, which can be caused by contact lens use, laser eye surgery, or nerve damage
Yet the consistent production of tears is critical to eye health. Tears serve to lubricate and protect the delicate surface of the eyes, and decreased tear production can lead to the following more serious complications:
- Eye inflammation
- Corneal abrasion and ulcers
- Damage to the ocular surface
- Eye infections
- Decreased quality of life such that daily activities are difficult or impossible1
Considering the potential risks of chronic dry eyes, finding safe and effective treatments for your patients is critical. Sometimes, removing the cause of a patient’s dry eyes is a simple solution – for example, discontinuing the offending medication or correcting the Vitamin A deficiency. Other times, however, a solution is more complex.
Current available treatment options for dry eyes include:
- Drugs like antibiotics and corticosteroids (taken orally or as eye drops) to reduce inflammation
- Eye inserts that work like artificial tears
- Drugs like cholinergics to increase tear production2
However, each of these treatment options has negative side effects. Antibiotics can negatively alter the microbiome and is a short-term solution at best. Corticosteroids suppress the immune system. Eye inserts can be quite uncomfortable for the patient, and cholinergics have a long list of side effects and contraindications.3
Platelet-rich plasma can be an excellent alternative to these treatments and has demonstrated safety and effectiveness in treating dry eye disease.
Studies show that topical PRP eye drops can be used to treat moderate to severe cases of dry eye disease that do not respond to conventional treatment.4 PRP has also been used for ocular surface surgical reconstruction.5
Platelet-Rich Plasma for Ophthalmic Concerns

Platelet-rich plasma, or PRP, is being used in ophthalmic settings to help heal the delicate tissues in the eyes. Rather than artificially suppressing inflammation or increasing tear production, PRP uses the body’s own natural healing process to regenerate damaged cells and tissue within the eyes.
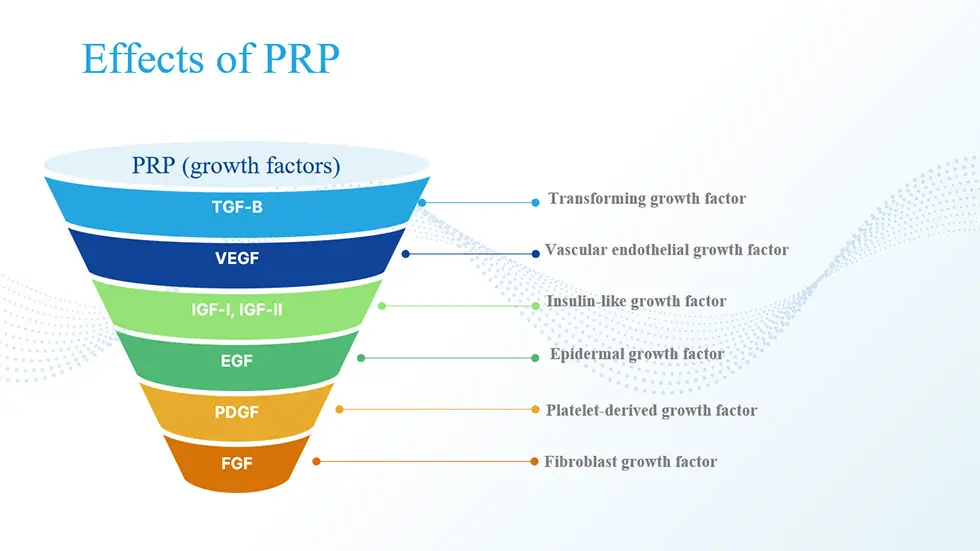
But how does it work? PRP stimulates the body’s innate healing cascade. When we experience an injury, our body responds by delivering a rush of platelet cells. When these platelets are activated, they release several types of growth factors, proteins, and cytokines that play a fundamental role in cell regeneration and tissue healing.
But PRP takes the natural healing response one step further by separating platelets from other blood components and concentrating them. This specially prepared platelet-rich plasma contains 5 to 10 times the concentration of platelets found in whole blood. The concentrated PRP is then delivered topically to the eyes as eye drops, stimulating and significantly strengthening the body’s healing response.6
Since PRP is an autologous therapy, using the patient’s own blood product, there is no risk of cross reactivity, disease transmission, or immune reaction.
THE PRP PROCESS
To create a platelet-rich plasma preparation, the following steps are performed:
- A small sample of blood is drawn from the patient and injected into the Dr. PRP blood tube.
- The platelets are then separated from the other blood components and their concentration is increased using the Dr. PRP centrifuge and by removing some of the plasma.
- The resulting platelet-rich plasma is then applied onto and around the injured site of the patient.
- The concentrated growth factors contained in the plasma trigger a mild inflammatory response which effectively jump starts the body’s own natural healing response.
The entire process takes approximately one hour, including preparation and recovery time. For a complete demonstration of each step of the process, view our instructional video.

DR. PRP
The Dr. PRP is an FDA-cleared medical device, holding the esteemed 510K clearance, meticulously designed to prepare patients' blood for PRP therapy quickly and efficiently.
Our patented design creates high-concentration and high-quality platelet-rich plasma that can be used by your physician to stimulate the healing process. This may result in tissue regeneration at the injured site, effectively accelerating normal healing processes.
REACH OUT TO LEARN MOREBENEFITS OF DR. PRP
SAFETY- Completely closed, sterile system.
- Outside air is blocked with a double safety cap.
- Since the processing is completed within the closed system, there is no risk of the PRP becoming contaminated.
- Each kit comes pre-packaged.
- The clear chambers ensure that you can see all the components of the blood sample.
- The buffy coat layer is easily seen in the neck of the device, allowing you to precisely separate the components into the type of PRP you wish to produce.
- You can even eliminate red blood cells from your final PRP product.
- The closed system allows for more treatments in less time.
- Customize your final PRP composition for use in different situations.
- The PRP can and should be administered as soon as you prepare it with our kit – no advanced preparation is needed.
- One kit holds 20 cc of fluid (3 cc of anticoagulant + 17 cc of whole blood) and produces 4 cc of highly concentrated PRP or 10 cc of a lower concentration.
- The platelet recovery percentage of Dr. PRP is higher than the minimal recovery percentage of other similar products from our competitors.
- Platelets require red and white blood cells to survive long-term. Unlike gel separators that capture the platelets within the gel, our kit allows you to accurately create consistently efficient PRP at the concentrations you desire.
- Our kit can recover over 90% of platelets from a blood sample to produce the highest quality PRP.
- The kit is now proudly holding the FDA 510K clearance.
- According to the ISO 13485, our kit is made with a thorough gamma-ray sterilization system.
- Made only with biocompatibility-certification completed raw materials.
- One-on-one, in-service training is provided via GoToTraining, FaceTime, or Zoom.
- User Manual with photos and descriptions detail how to use your new product, as well as information on PRP and test results.
- Enroll in our Platelet-Rich Plasma CME Certification course where you can learn cosmetic applications of PRP, including the PRP Facial and PRP Facelift.
- Order marketing materials and educational brochures for your patients. These brochures explain various applications of PRP, such as sports medicine and hair regeneration.
- Add your contact information and location to our Directory of PRP Providers.
To view and order Dr. PRP kits and centrifuges, visit our online store. For questions and to discuss our products in more detail, contact us today at 844-377-7787 (DR- PRP-US).
References
- “Dry Eyes: Symptoms & causes.” Mayo Clinic. Accessed June 24, 2021. https://www.mayoclinic.org/diseases-conditions/dry-eyes/symptoms-causes/syc-20371863
- “Dry Eyes: Diagnosis & treatment.” Mayo Clinic. Accessed June 24, 2021. https://www.mayoclinic.org/diseases-conditions/dry-eyes/diagnosis-treatment/drc-20371869
- Pakala RS, Brown KN, Preuss CV. Cholinergic Medications. [Updated 2021 Feb 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538163/
- https://www.researchgate.net/publication/325190146_The_Use_of_Platelet-Rich_Plasma_in_Dry_Eye_Disease
- Alio JL, Rodriguez AE, Wróbel-Dudzińska D. “Eye platelet-rich plasma in the treatment of ocular surface disorders.” Current Opinion in Ophthalmology. 2015 Jul;26(4):325-32. doi: 10.1097/ICU.0000000000000169. PMID: 26058033.
- “PRP Injections for Pain.” American Academy / Association of Orthopedic Medicine. Accessed June 24, 2021. https://www.aaomed.org/Platelet-Rich-Plasma-Injections-for-Pain


